Post-stent chest pain, revisited
Heart Sisters
JULY 28, 2024
Heart patients with persistent or recurrent post-stent chest pain present “an unmet clinical need”, according to the European Journal of Cardiology.
This site uses cookies to improve your experience. To help us insure we adhere to various privacy regulations, please select your country/region of residence. If you do not select a country, we will assume you are from the United States. Select your Cookie Settings or view our Privacy Policy and Terms of Use.
Cookies and similar technologies are used on this website for proper function of the website, for tracking performance analytics and for marketing purposes. We and some of our third-party providers may use cookie data for various purposes. Please review the cookie settings below and choose your preference.
Used for the proper function of the website
Used for monitoring website traffic and interactions
Cookies and similar technologies are used on this website for proper function of the website, for tracking performance analytics and for marketing purposes. We and some of our third-party providers may use cookie data for various purposes. Please review the cookie settings below and choose your preference.

Heart Sisters
JULY 28, 2024
Heart patients with persistent or recurrent post-stent chest pain present “an unmet clinical need”, according to the European Journal of Cardiology.
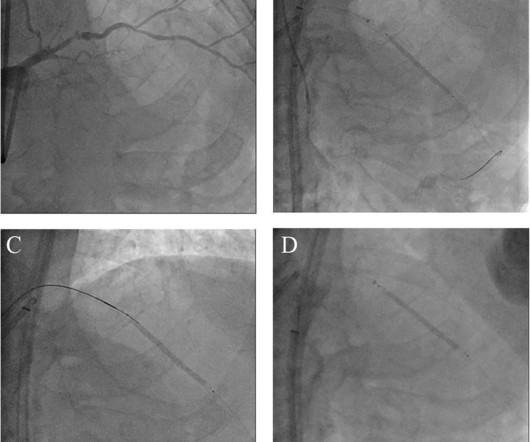
Frontiers in Cardiovascular Medicine
MARCH 16, 2025
BackgroundAn undeflatable stent balloon following its inflation during percutaneous coronary intervention (PCI) is a rare and unpredictable complication that can lead to serious consequences. Currently, there is no standardized protocol for managing this issue.Case presentationAn 83-year-old man presented with chest pain.
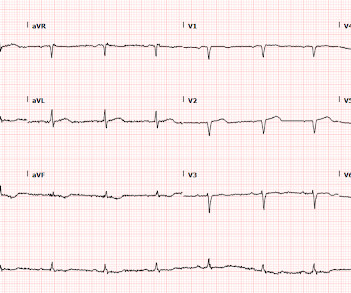
Dr. Smith's ECG Blog
MAY 29, 2024
Written by Pendell Meyers Two patients with acute chest pain. Patient 1: Patient 2: Patient 1: A man in his 40s with minimal medical history presented with acute chest pain radiating to his R shoulder. Two patients with chest pain. Do either, neither, or both have OMI and need reperfusion?

Dr. Smith's ECG Blog
MARCH 19, 2024
The patient presented to an outside hospital An 80yo female per triage “patient presents with chest pain, also hurts to breathe” PMH: CAD, s/p stent placement, CHF, atrial fibrillation, pacemaker (placed 1 month earlier), LBBB. HPI: Abrupt onset of substernal chest pain associated with nausea/vomiting 30 min PTA.
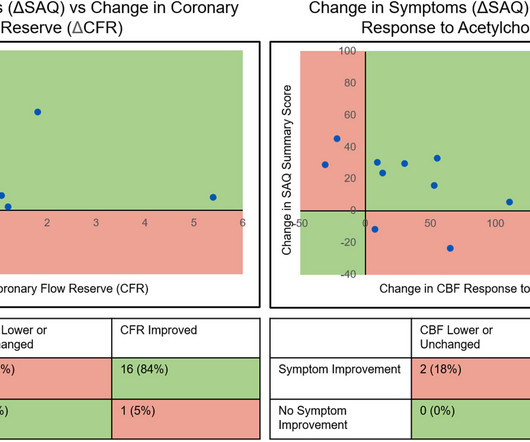
Medical Xpress - Cardiology
NOVEMBER 7, 2024
A study at Mayo Clinic suggests that an hourglass-shaped stent could improve blood flow and ease severe and reoccurring chest pain in people with microvascular disease. Of 30 participants in a phase 2 clinical trial, 76% saw improvement in their day-to-day life.
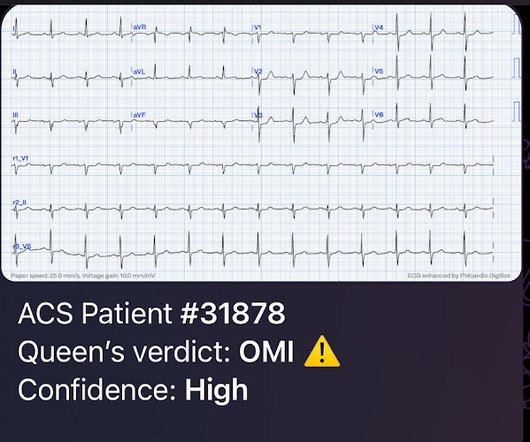
Dr. Smith's ECG Blog
MARCH 31, 2024
The patient was a middle-aged female who had acute chest pain of approximately 6 hours duration. The pain was still active at the time of evaluation. Angiogram reportedly showed acute thrombotic occlusion of the first obtuse marginal which was stented. Peak troponin was not recorded. Long term follow up is unavailable.
Dr. Smith's ECG Blog
SEPTEMBER 11, 2024
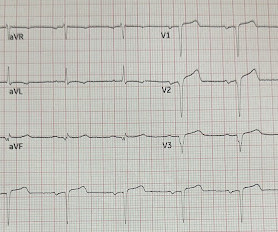
No Chest Pain, but somnolent. The fact that this is syncope makes give it a far lower pretest probability than chest pain, but it was really more than syncope, as the patient actually underwent CPR and had hypotension on arrival of EMS. Former resident: "Just saw cath report, LAD stent was 100% acutely occluded."
Dr. Smith's ECG Blog
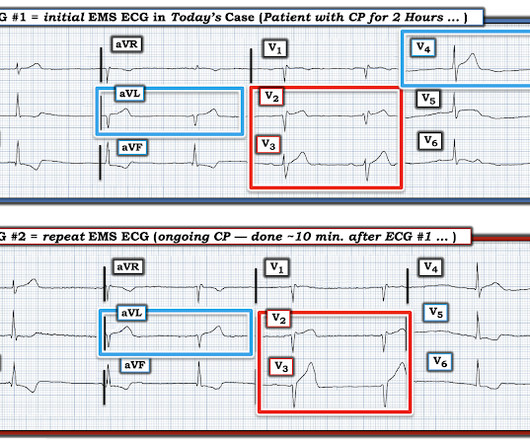
AUGUST 11, 2024
Written by Jesse McLaren A healthy 75 year old developed 7/10 chest pain associated with diaphoresis and nausea, which began on exertion but persisted. Below is the first ECG recorded by paramedics after 2 hours of chest pain, interpreted by the machine as “possible inferior ischemia”. What do you think?

Dr. Smith's ECG Blog
APRIL 14, 2024
A 56 year old male with PMHx significant for hypertension had chest pain for several hours, then presented to the ED in the middle of the night. He reported chest pain that developed several hours prior to arrival and was 5/10 in intensity. The pain was located in the mid to left chest and developed after riding his bike.

Dr. Smith's ECG Blog
APRIL 22, 2024
A 50-something male with hypertension and 20- to 40-year smoking history presented with 1 week of stuttering chest pain that is worse with exertion, which takes many minutes to resolve after resting and never occurs at rest. At times the pain does go to his left neck. It is a ssociated with mild dyspnea on exertion.
Dr. Smith's ECG Blog
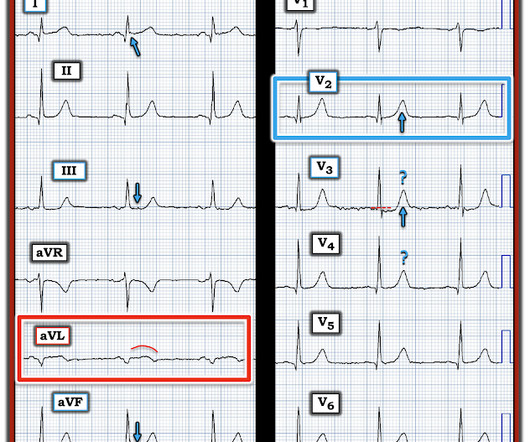
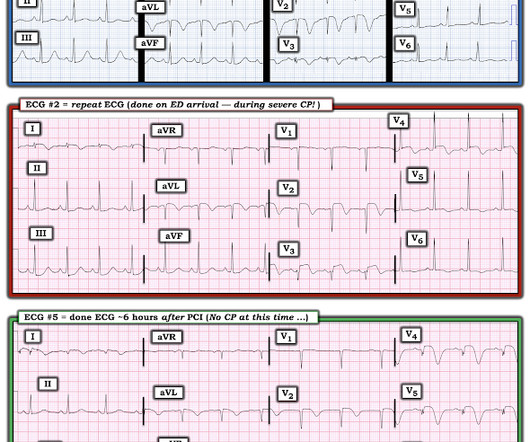
AUGUST 6, 2024
Written by Magnus Nossen with Edits by Grauer and Smith The ECGs in today’s case are from 3 different patients all presenting with new-onset CP ( Chest Pain ). As a result, this 45-year old man did not experince any delay in treatment — and a large diagonal branch of the LAD was stented with good outcome.
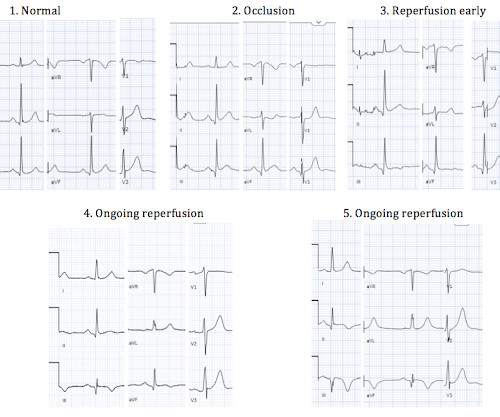
Dr. Smith's ECG Blog
JANUARY 27, 2024
Written by Jesse McLaren, comments by Smith A 55 year old with a history of NSTEMI presented with two hours of exertional chest pain, with normal vitals. Old ‘NSTEMI’ A history of coronary artery disease and a stent to the same territory further increases pre-test likelihood of acute coronary occlusion, including in-stent thrombosis.
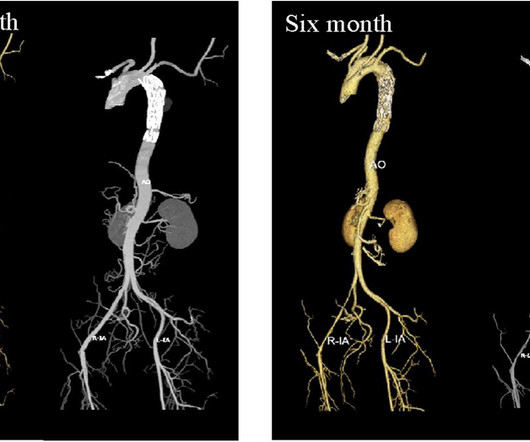
Frontiers in Cardiovascular Medicine
DECEMBER 5, 2024
Follow-up CTA scans at one- and six-month post-operation showed that the aortic stent was well-positioned, with no visible primary lesion.
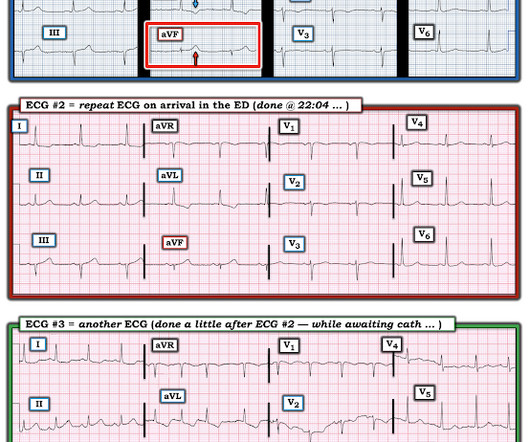
Dr. Smith's ECG Blog
JULY 23, 2024
I was working at triage when the medics brought this patient who is 65 yo and has had chest pain for 12 hours. It was opened and stented. They recorded a prehospital ECG at 2112 and said that it was “normal”. It had already been crumpled up and put in the waste basket. So I uncrumpled it: What do you think?

Dr. Smith's ECG Blog
MARCH 22, 2024
Written by Willy Frick A man in his 50s with history of hypertension, hyperlipidemia, and a 30 pack-year smoking history presented to the ER with 1 hour of acute onset, severe chest pain and diaphoresis. His ECG is shown: What do you think? What do you think? This was the cost of preventing infarction of the anterior wall.)
Med Page Today
MARCH 5, 2024
(MedPage Today) -- FDA approved the Agent drug-coated balloon (DCB) for coronary in-stent restenosis, making this the first DCB to make it to the U.S. In people with stable chest pain, a coronary. market, manufacturer Boston Scientific announced.

Dr. Prateek Bhatnagar
MAY 11, 2022
A 55 years old diabetic male patient who had 12 stents in his heart underwent a successful beating heart bypass surgery under Dr. Prateek Bhatnagar, Director Cardiac Surgery. The patient was suffering with angina (chest pain) since 2002. The last 3 stents were placed just 6 months back but were not working.

Dr. Prateek Bhatnagar
SEPTEMBER 6, 2023
Prateek Bhatnagar Director Cardiac Surgery, on a 50 years man after stents placed in his left main coronary artery at Delhi just 3 months back, had blocked. Mr. Hemant, a resident of Delhi NCR, had developed chest pain (angina). He subsequently underwent stenting procedure in left main coronary artery.
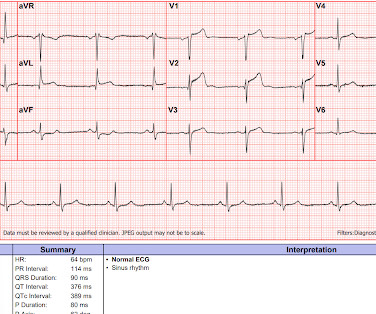
Dr. Smith's ECG Blog
MAY 23, 2023
Written by Pendell Meyers A man in his early 40s experienced acute onset chest pain. The chest pain started about 24 hours ago, but there was no detailed information available about whether his pain had come and gone, or what prompted him to be evaluated 24 hours after onset.
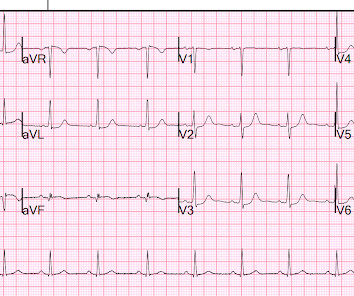
Dr. Smith's ECG Blog
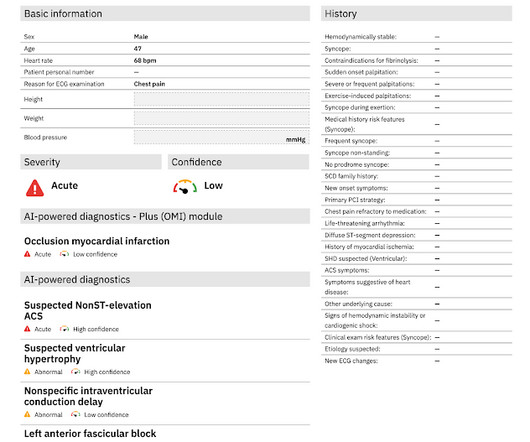
JUNE 5, 2023
A 40-something male presented by ambulance with one hour of chest pain that was improving after sublingual nitroglycerine and 325 mg of aspirin, chewed. It must have re-occluded between the ED and the cath lab) --Lesion was stented. Here is his initial ED ECG: What do you think?
Dr. Smith's ECG Blog
JANUARY 25, 2024
A 40-something with severe diabetes on dialysis and with known coronary disease presented with acute crushing chest pain. The pain did not resolve with NTG, and so he went to emergent angiography: 1. LAD: severe in-stent restenosis in the mid (80%) and distal (90%) segment and diffuse disease distally.

Dr. Smith's ECG Blog
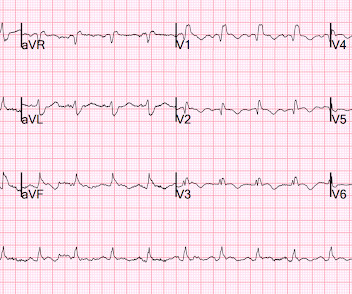
DECEMBER 29, 2023
Written by Jesse McLaren A previously healthy 50 year-old presented with 24 hours of intermittent exertional chest pain, radiating to the arms and associated with shortness of breath. In a previously healthy patient with new and ongoing chest pain, this is concerning for acute occlusion of the first diagonal artery.
Dr. Smith's ECG Blog
NOVEMBER 17, 2023
It is of an elderly woman who complained of shortness of breath and had a recent stent placed. Also, we know the patient had a stent. Finally, the presentation is dyspnea, not chest pain. A few days before that, she had had an LAD stent for LAD occlusion. I was texted this ECG just as I was getting into bed.

Dr. Smith's ECG Blog
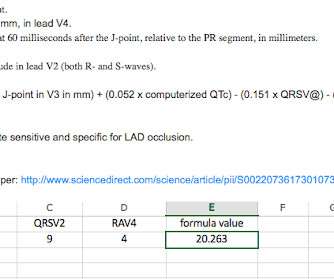
FEBRUARY 6, 2023
Sent by anonymous, written by Pendell Meyers A man in his 60s presented with acute chest pain with diaphoresis. The Importance of the History: As noted above — the onset of chest pain in today's case was acute. He had received aspirin and nitroglycerin by EMS, with some improvement. His vitals were within normal limits.
Dr. Smith's ECG Blog
OCTOBER 3, 2017
This is another case written by Pendell Meyers (who is helping to edit the blog and has many great recent posts) Case A 45 year old man was driving to work when he experienced acute onset sharp left sided chest pain with paresthesias of the left arm. A repeat ECG was recorded with pain 2/10: Not much change.
Dr. Smith's ECG Blog
MARCH 13, 2023
A 40-something woman called 911 in the middle of the night for Chest pain that was intermittent. On arrival, she complained of severe pain. The medics had recorded this ECG and were uncertain whether it was recorded during chest pain: Let's get a better image with use of the PM Cardio app : What do you think?
Dr. Smith's ECG Blog
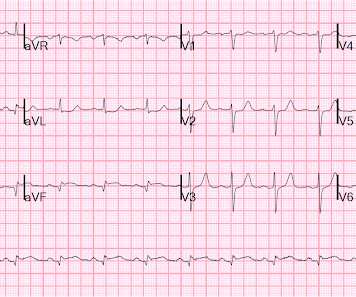
APRIL 12, 2013
A male in his 40's who had been discharged 6 hours prior after stenting of an inferoposterior STEMI had sudden severe SOB at home 2 hours prior to calling 911. He had no chest pain. Medications were aspirin, clopidogrel, metoprolol, and simvastatin. He was in acute distress from pulmonary edema, with a BP of 180/110, pulse 110.

Dr. Smith's ECG Blog
MAY 30, 2023
A 50-something man presented in shock with severe chest pain. Angiogram: Culprit Lesion (s): Thrombotic occlusion of the proximal RCA -- stented. His prehospital ECG was diagnostic of inferior posterior OMI. The patient was in clinical shock with a lactate of 8. He appeared gray in color, with cool skin.
Dr. Smith's ECG Blog
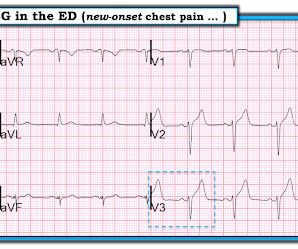
MAY 11, 2019
male was sitting at a work conference when he began having substernal chest pain with diaphoresis. The pain was 7 out of 10 when this ECG was recorded: The QTc = 375 What do you think? Here is the post stent ECG: This is probably the amount of ST elevation (zero) that this patient has at baseline.
Dr. Smith's ECG Blog
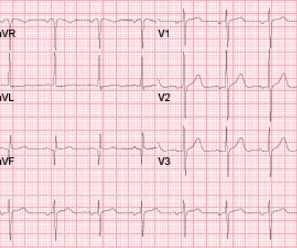
JANUARY 6, 2023
Submitted and written by Anonymous, edits by Meyers and Smith A 50s-year-old patient with no known cardiac history presented at 0045 with three hours of unrelenting central chest pain. The pain was heavy, radiated to her jaw with an associated headache. A single DES stent was placed, and the patient did well post-procedure.
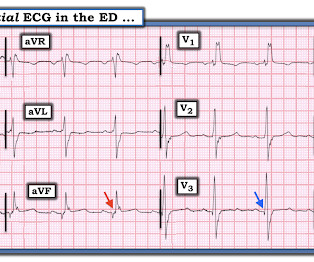
Dr. Smith's ECG Blog
JANUARY 31, 2020
The patient's chest pain had resolved by the time of the ECG 2. But it does prove that the patient has coronary disease and makes the probability that his chest pain is due to ACS very very high. Angiogram: Widely patent RCA and LAD stents. Therefore, no stent was placed. (No There are well-formed Q-waves 3.

Dr. Smith's ECG Blog
APRIL 14, 2023
Sent by Anonymous, written by Pendell Meyers A man in his 60s with history of CAD and 2 prior stents presented to the ED complaining of acute heavy substernal chest pain that began while eating breakfast about an hour ago, and had been persistent since then, despite EMS administering aspirin and nitroglycerin. Pre-intervention.
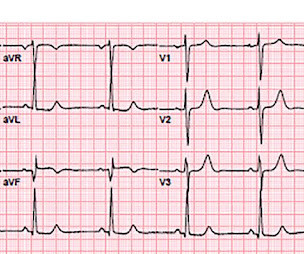
Dr. Smith's ECG Blog
NOVEMBER 26, 2015
52-year-old lady presents to the Emergency Department with 2 hours of chest pain, palpitations & SOB. Without them the diagnosis is often tough and one must often rely on other clinical data- serial ECG’s, troponin, on-going chest pain, etc. She received PCI with 2 drug-eluting stents in overlying fashion.
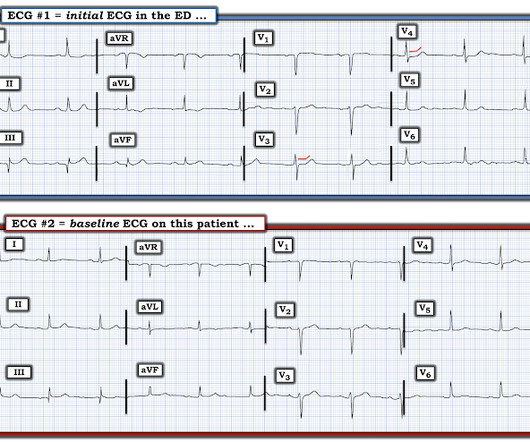
Dr. Smith's ECG Blog
NOVEMBER 23, 2022
Case submitted by Rachel Plate MD, written by Pendell Meyers A man in his 70s presented with chest pain which had started acutely at rest and has lasted for 2 hours. The pain was still ongoing at arrival. He also noted a bilateral "odd feeling" in his arms. He stated it was similar to prior heart attacks.

DAIC
APRIL 8, 2024
The study focused on patients who underwent PCI for acute coronary syndromes (ACS)—life-threatening conditions which include heart attacks and chest pain caused by decreased blood flow to the heart—with stents containing drugs to prevent further plaque buildup. Stents were supplied by Medtronic Corp. Minnesota, U.S.)
Dr. Smith's ECG Blog
DECEMBER 14, 2016
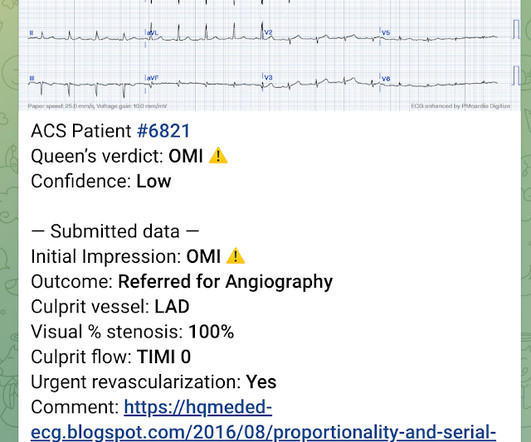
A middle aged male presented at midnight after 14 hours of constant, severe substernal chest pain, radiating to his throat and to bilateral jaws, and associated with diaphoresis. The pain was not positional, pleuritic, or reproducible. It was not relieved by anything. He had no previous medical history.
Dr. Smith's ECG Blog
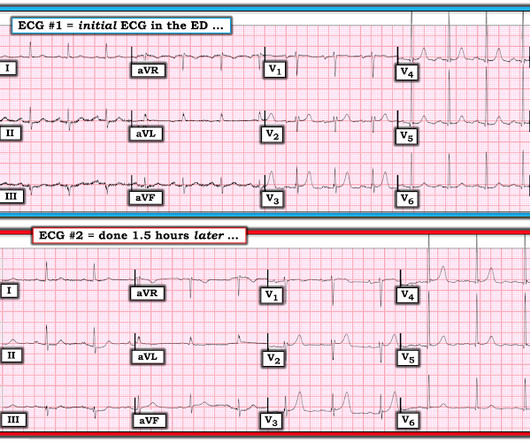
SEPTEMBER 29, 2023
A 60-something woman called EMS for chest pain. link] Clinical Course I don't know if the medics noticed these ECG findings or not, but if not, they recognized the value of serial ECGs in a patient with chest pain. The medics administered aspirin (no Nitroglycerine), and the pain resolved. #5: mm in V2 and 0.65
Dr. Smith's ECG Blog
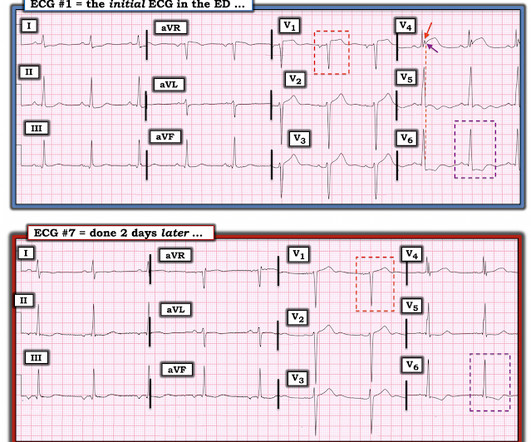
SEPTEMBER 27, 2019
An elderly woman presented with chest pain that radiated to the back for several hours. The first troponin returned at 0.099 ng/mL (elevated, consistent with Non-Occlusion MI) Providers were concerned with aortic dissection, so they order a chest aorta CT. Here is here initial ECG: There is only a nonspecific flat T-wave in aVL.
Dr. Smith's ECG Blog
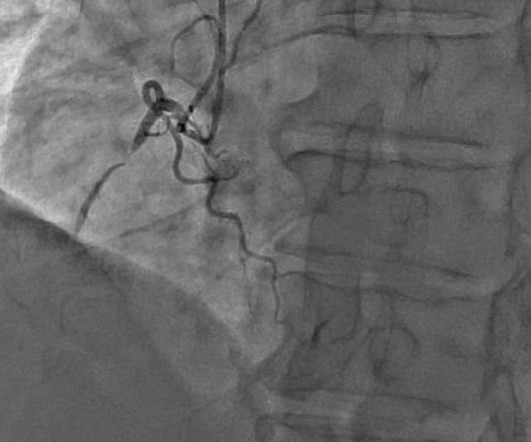
NOVEMBER 1, 2022
The 50-something patient with history of coronary stenting and slightly reduced LV ejection fraction. In the setting of prior stenting and reduced left ventricular ejection fraction, would pursue a heart team revascularization approach Syntax score 28.5, Pericarditis would be even more unlikely in someone without chest pain.
Dr. Smith's ECG Blog
SEPTEMBER 30, 2019
Case written and submitted by Ryan Barnicle MD, with edits by Pendell Meyers While vacationing on one of the islands off the northeast coast, a healthy 70ish year old male presented to the island health center for an evaluation of chest pain. The chest pain started about one hour prior to arrival while bike riding.
Dr. Smith's ECG Blog
JULY 11, 2019
Written and submitted by Ashley Mogul, with edits by Pendell Meyers and Steve Smith A man in his 40s with recent smoking cessation but otherwise no known past medical history presented due to chest pain since the previous evening. The pain has been constant and associated with vomiting and diaphoresis.
Dr. Smith's ECG Blog
OCTOBER 1, 2023
A man in his mid 60s with history of CAD and stents experienced sudden onset epigastric abdominal pain radiating up into his chest at home, waking him from sleep. He had active chest pain at the time of triage at 0137 at night, with this triage ECG: What do you think? It is stented with good angiographic result.
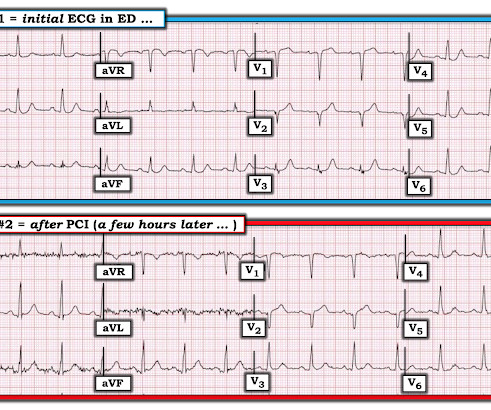
Dr. Smith's ECG Blog
MAY 20, 2024
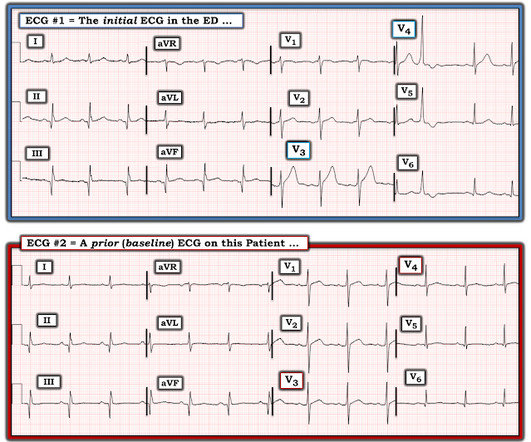
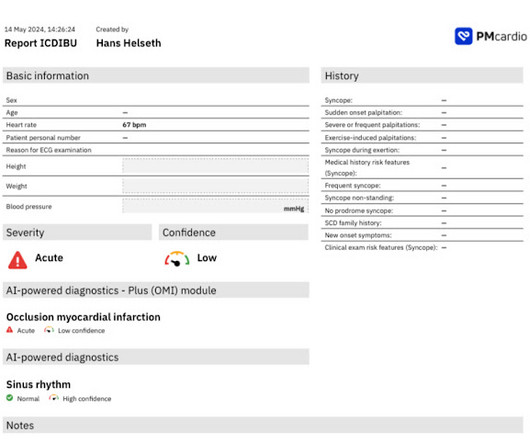
A 63 year old man with a history of hypertension, hyperlipidemia, prediabetes, and a family history of CAD developed chest pain, shortness of breath, and diaphoresis after consuming a large meal at noon. He called EMS, who arrived on scene about two hours after the onset of pain to find him hypertensive at 220 systolic.
Dr. Smith's ECG Blog
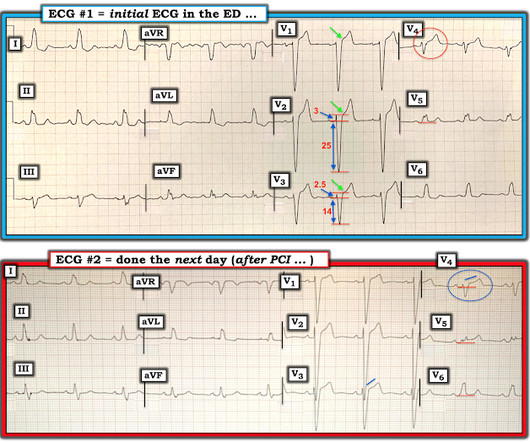
DECEMBER 16, 2019
A 50-something male who is healthy and active with no previous medical history presented with 5 hours of continuous worrisome chest pain. Chest pain with New LBBB: It helps to actually measure the ST/S ratio A Fascinating Demonstration of ST/S Ratio in LBBB and Resolving LAD Ischemia The cath lab was activated.
Expert insights. Personalized for you.
We have resent the email to
Are you sure you want to cancel your subscriptions?


Let's personalize your content