ECG Cases 48 – ECG Interpretation in Cardiac Arrest
ECG Cases
FEBRUARY 13, 2024
The post ECG Cases 48 – ECG Interpretation in Cardiac Arrest appeared first on Emergency Medicine Cases.
This site uses cookies to improve your experience. To help us insure we adhere to various privacy regulations, please select your country/region of residence. If you do not select a country, we will assume you are from the United States. Select your Cookie Settings or view our Privacy Policy and Terms of Use.
Cookies and similar technologies are used on this website for proper function of the website, for tracking performance analytics and for marketing purposes. We and some of our third-party providers may use cookie data for various purposes. Please review the cookie settings below and choose your preference.
Used for the proper function of the website
Used for monitoring website traffic and interactions
Cookies and similar technologies are used on this website for proper function of the website, for tracking performance analytics and for marketing purposes. We and some of our third-party providers may use cookie data for various purposes. Please review the cookie settings below and choose your preference.

ECG Cases
FEBRUARY 13, 2024
The post ECG Cases 48 – ECG Interpretation in Cardiac Arrest appeared first on Emergency Medicine Cases.
Ken Grauer, MD
JUNE 14, 2024
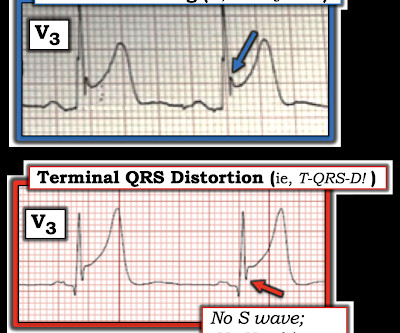
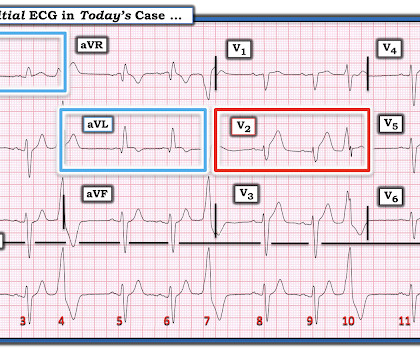
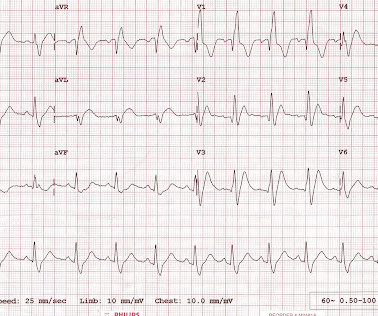
The ECG in Figure-1 — was obtained from a middle-aged man who presented to the ED ( E mergency D epartment ) in cardiac arrest. Prompt cath is therefore advised if the post-ROSC shows an acute STEMI. To Emphasize: The phenomenon of T-QRS-D is not needed in today's case to recognize the acute STEMI.

Ken Grauer, MD
FEBRUARY 3, 2024
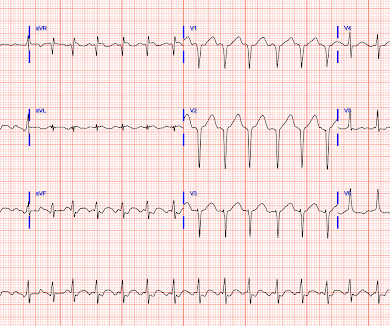
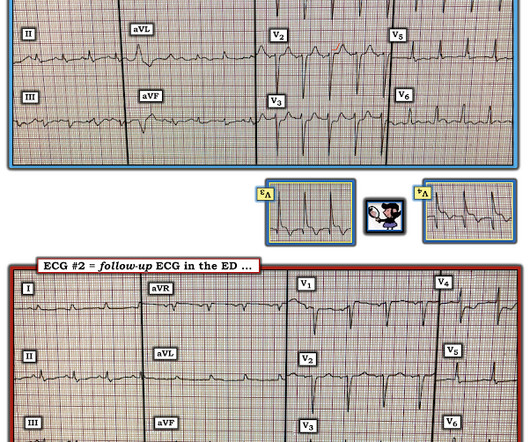
Shortly after arrival in the ED ( E mergency D epartment ) — she suffered a cardiac arrest. BUT — Cardiac catheterization done a little later did not reveal any significant stenosis. Figure-1: The initial ECG in today's case — obtained after successful resuscitation from cardiac arrest. ( No CP ( C hest P ain ).
Dr. Smith's ECG Blog
JULY 9, 2024
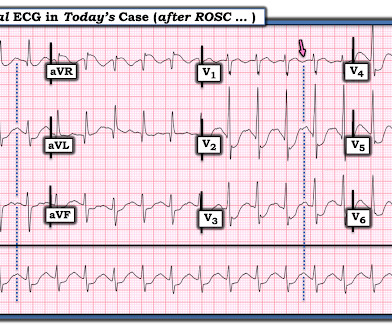
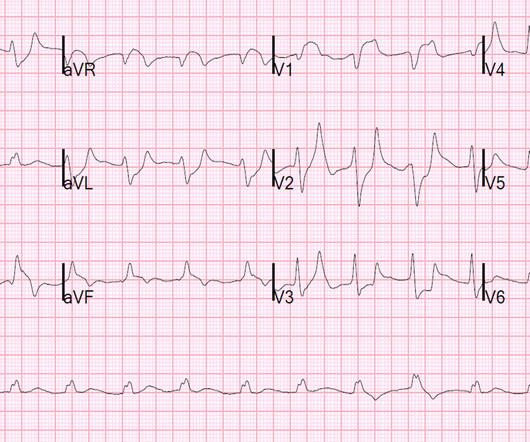
Written by Pendell Meyers A man in his 50s was found by his family in cardiac arrest of unknown duration. Despite anticipation by many that the initial post-resuscitation ECG will show an obvious acute infarction — this expected "STEMI picture" is often not seen. Restoration of sinus rhythm is evident in Figure-1.
Dr. Smith's ECG Blog
JULY 25, 2024
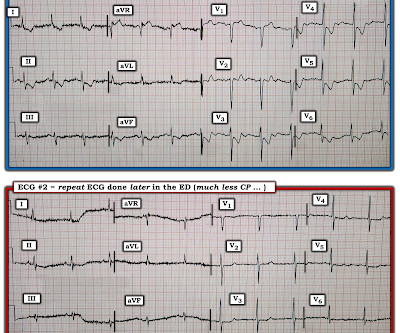
But cardiac arrest is a period of near zero flow in the coronary arteries and causes SEVERE ischemia. After cardiac arrest, I ALWAYS wait 15 minutes after an ECG like this and record another. See these related cases: Cardiac arrest, defibrillated, diffuse ST depression and ST Elevation in aVR.
Ken Grauer, MD
OCTOBER 21, 2023
PEARL # 1: Although seeing an elevated Troponin would provide additional support for immediate cardiac catheterization — the clinical reality is that the initial Troponin reading will not always be elevated in patients with acute coronary occlusion ( See March 24, 2023 post in Dr. Smith's ECG Blog ).
Dr. Smith's ECG Blog
JUNE 27, 2024
A patient had a cardiac arrest with ventricular fibrillation and was successfully defibrillated. COACT: The COACT trial was fatally flawed, and because of it, many cardiologists are convinced that if there are no STEMI criteria, the patient does not need to go to the cath lab. These studies did not address OMI ECG findings!!!

Dr. Smith's ECG Blog
SEPTEMBER 20, 2011
This 80 year old with a history of CABG had a cardiac arrest. This is as clear a STEMI as you can get. Now, it is true that shortly after a non-ACS cardiac arrest, there can be transient diffuse ST depression, but not ST elevation in a coronary distribution, and there should not be a wall motion abnormality.

Ken Grauer, MD
MAY 26, 2023
At some point ~1-2 hours after the initial ECG — the patient developed runs of VT, leading to cardiac arrest. ECG Blog #185 — Review of the P s, Q s, 3 R Approach for systematic rhythm interpretation. ECG Blog #271 — Reviews the concept of diffuse Subendocardial Ischemia. ECG Blog #316 — The patient died.

Ken Grauer, MD
JUNE 6, 2023
== P lease N OTE : After today — No new ECG Blog posts for 2- to -3 weeks. — I will also not be prompt in replying to emails. == All material on this ECG Blog site remains open! IF you scroll down a little on the right-hand column of this blog — You'll see a lot of icons. Figure-1: The initial ECG in today's case.

Dr. Smith's ECG Blog
FEBRUARY 22, 2024
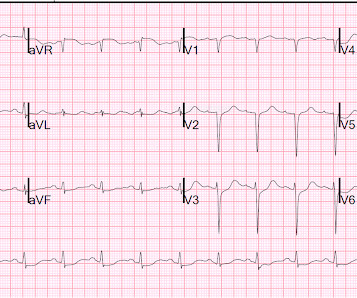
A woman in her 50s with dyspnea and bradycardia A patient with cardiac arrest, ROSC, and right bundle branch block (RBBB). HyperKalemia with Cardiac Arrest. Peaked T waves: Hyperacute (STEMI) vs. Early Repolarizaton vs. Hyperkalemia What will you do for this altered and bradycardic patient?
Dr. Smith's ECG Blog
OCTOBER 20, 2013
Note that they finally have laid to rest the new or presumably new LBBB as a criteria for STEMI. Note that they finally have laid to rest the new or presumably new LBBB as a criteria for STEMI. Also note that they allow ST depression c/w posterior MI to be a STEMI equivalent. What is the utility of a head CT in cardiac arrest?
Dr. Smith's ECG Blog
SEPTEMBER 29, 2024
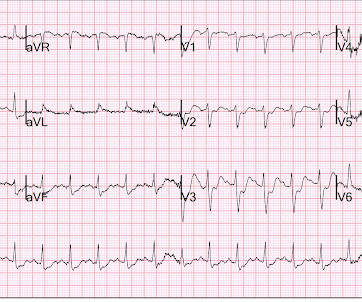
This certainly looks like an anterior STEMI (proximal LAD occlusion), with STE and hyperacute T-waves (HATW) in V2-V6 and I and aVL. How do you explain the anterior STEMI(+)OMI immediately after ROSC evolving into posterior OMI 30 minutes later? This caused a type 2 anterior STEMI.

Dr. Smith's ECG Blog
APRIL 24, 2015
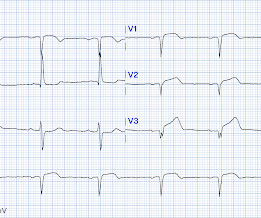
ST depression is common BOTH after resuscitation from cardiac arrest and during atrial fib with RVR. Again, it is common to have an ECG that shows apparent subendocardial ischemia after resuscitation from cardiac arrest, after defibrillation, and after cardioversion. The patient was cardioverted. This was done.
Dr. Smith's ECG Blog
OCTOBER 8, 2024
Subtle as a STEMI." (i.e., About 45 minutes after the second EKG, the patient was found in cardiac arrest. Later the next day, she went into cardiac arrest again. By the time I saw the repeat EKG, the patient was already in cardiac arrest. None of the 20 ever evolved to STEMI criteria.
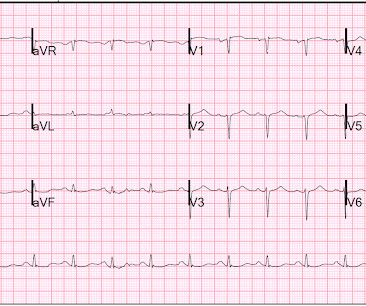
Dr. Smith's ECG Blog
OCTOBER 28, 2013
The last section is a detailed discussion of the research on aVR in both STEMI and NonSTEMI. The additional ST Elevation in V1 is not usually seen with diffuse subendocardial ischemia, and suggests that something else, like STEMI from LAD occlusion, could be present. Here is an article I wrote: Updates on the ECG in ACS. see below).
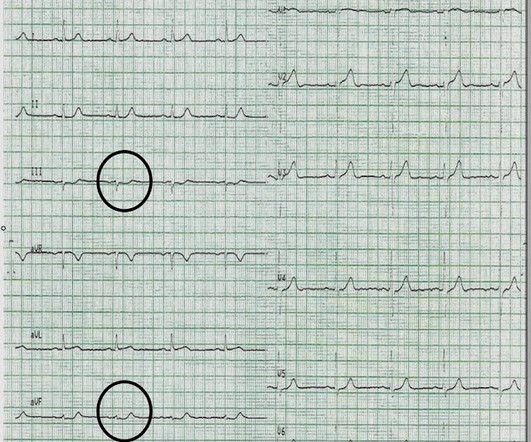
Dr. Smith's ECG Blog
OCTOBER 24, 2013
Appreciation of these subtle ECG findings could have helped to avoid a cardiac arrest and its resulting permanent disability 3. Ischemia on the ECG can be very subtle and is easily missed. Accurate interpretation requires a lot of skill, practice, and experience.
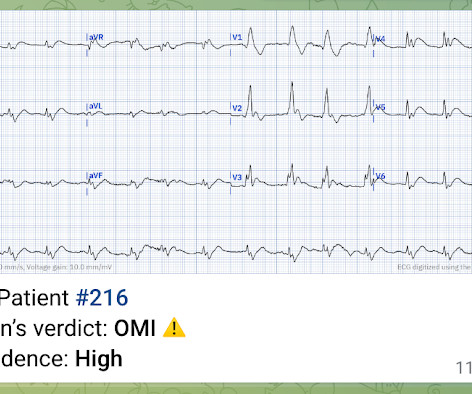
Dr. Smith's ECG Blog
JULY 14, 2023
Two recent interventions have proven in randomized trials to improve neurologic survival in cardiac arrest: 1) the combination of the ResQPod and the ResQPump (suction device for compression-decompression CPR -- Lancet 2011 ) and 2) Dual Sequential defibrillation. First — Some thoughts on the post -resuscitation ECG.

Dr. Smith's ECG Blog
JUNE 21, 2023
You can subscribe for news and early access (via participating in our studies) to the Queen of Hearts here: [link] queen-form This EMS ECG was transmitted to the nearby Emergency Department where it was remotely reviewed by a physician, who interpreted it as normal, or at least without any features of ischemia or STEMI.
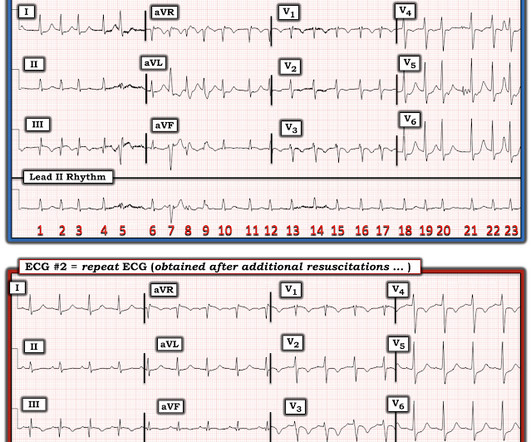
Dr. Smith's ECG Blog
OCTOBER 10, 2022
He had multiple cardiac arrests with ROSC regained each time. Then there is loss of pulses with continued narrow complex on the monitor ("PEA arrest") Learning Points: Sudden witnessed Cardiac Arrest due to ACS is almost always due to dysrhythmia. This patient arrested shortly after hospital arrival.
Dr. Smith's ECG Blog
APRIL 8, 2016
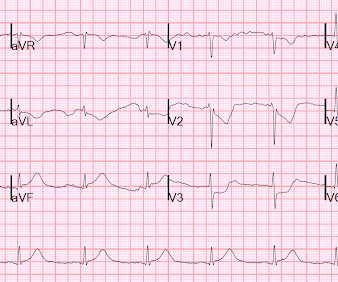
Here is his ED ECG: There is obvious infero-posterior STEMI. What are you worried about in addition to his STEMI? Comments: STEMI with hypokalemia, especially with a long QT, puts the patient at very high risk of Torsades or Ventricular fibrillation (see many references, with abstracts, below). There is atrial fibrillation.
Dr. Smith's ECG Blog
NOVEMBER 12, 2020
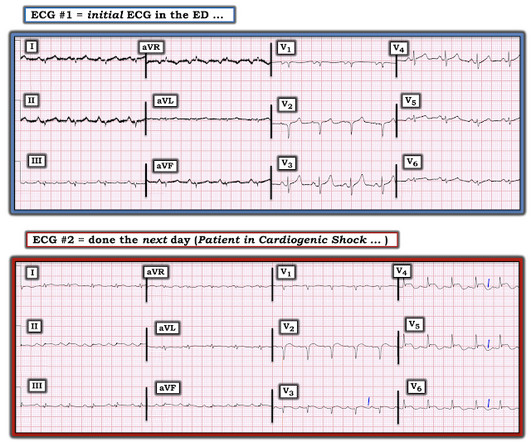
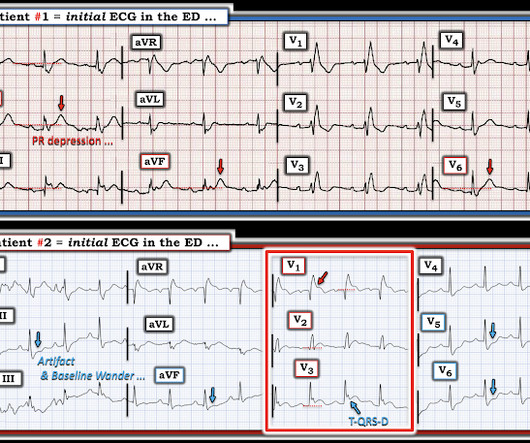
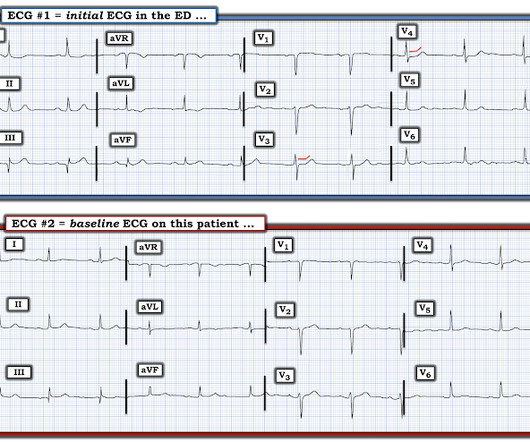
In a series of 18 patients with COVID and ST elevation, 8 were diagnosed with STEMI, 6 of whom had an angiogram and it showed obstructive coronary disease. 12 All STEMI patients had very high cTn typical of STEMI (cTnT > 1.0 POINT #2: Overall QRS amplitude ( voltage ) is dramatically reduced in ECG #1.
Dr. Smith's ECG Blog
SEPTEMBER 21, 2020
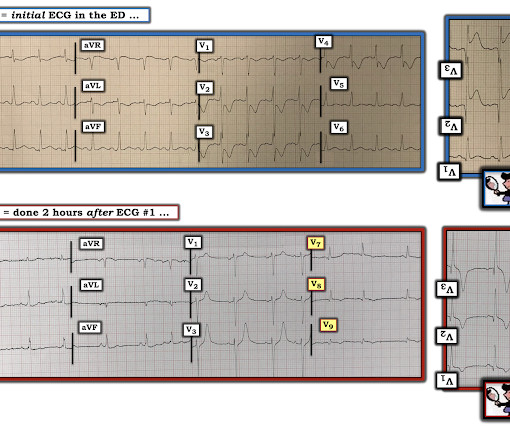
Are Some Cardiologists Really Limited by Strict Adherence to STEMI millimeter criteria? I was texted these ECGs by a recent residency graduate after they had all been recorded, along with the following clinical information: A 50-something with no cardiac history, but with h/o Diabetes, was doing physical work when he collapsed.
Dr. Smith's ECG Blog
JANUARY 25, 2017
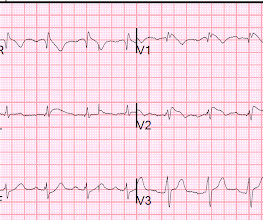
911 was called and the medics recorded this ECG (unfortunately, leads V4-V6 are missing) Due to marked ST Elevation, the computer read was STEMI What do you think? See this post and associated case reports: Cardiac arrest, severe acidosis, and a bizarre ECG The patient was admitted and ruled out for acute MI by serial troponins.
Dr. Smith's ECG Blog
OCTOBER 4, 2010
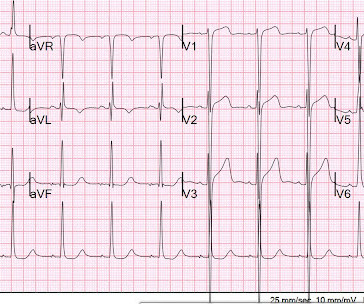
Thus, this patient had increased ST elevation (current of injury) superimposed on the ST elevation of LVH and simulating STEMI. The stress of the triathlon cause demand ischemia and ventricular fibrillation. He awoke and did well.
Dr. Smith's ECG Blog
NOVEMBER 28, 2018
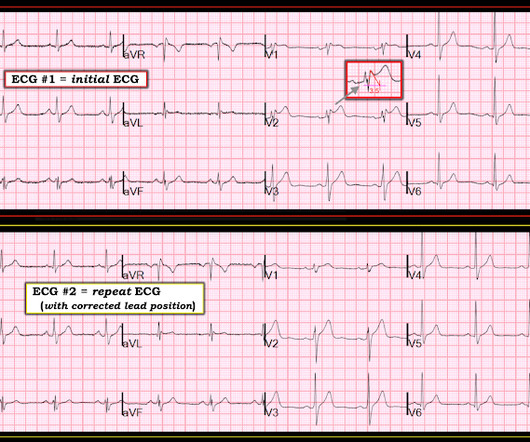
Saddleback ST Elevation is almost never STEMI 2. An inverted P-wave in lead V2 implies lead misplacement too high Saddleback in STEMI: Here are the only 2 ECGs with V2 "saddleback" that I have ever seen which really represented an LAD Occlusion: Anatomy of a Missed LAD Occlusion (classified as a NonSTEMI) A Very Subtle LAD Occlusion.T-wave
Dr. Smith's ECG Blog
AUGUST 19, 2023
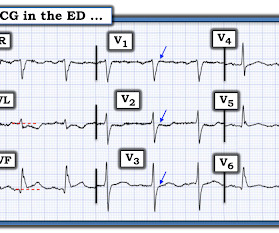
This is diagnostic of infero-posterior OMI, but it is falsely negative by STEMI criteria and with falsely negative posterior leads (though they do show mild ST elevation in V4R). They were less likely to have STEMI on ECG, and more likely to be initially diagnosed as non-ACS.
Dr. Smith's ECG Blog
OCTOBER 25, 2023
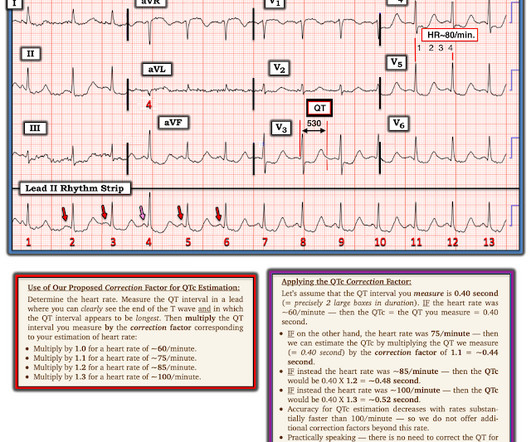
Polymorphic Ventricular Tachycardia Long QT Syndrome with Continuously Recurrent Polymorphic VT: Management Cardiac Arrest. A New Seizure in a Healthy 20-something More cases of long QT not measured correctly by computer (these are all fascinating ECGs/cases): Bupropion Overdose Followed by Cardiac Arrest and, Later, ST Elevation.

Dr. Smith's ECG Blog
JULY 21, 2024
The ECG shows obvious STEMI(+) OMI due to probable proximal LAD occlusion. As we've often emphasized on Dr. Smith's ECG Blog — it is rare in practice to see LMCA occlusion, because most such patients die before reaching the hospital. The below ECG was recorded. Figure-1: I've labeled the initial ECG in today's case. (
Dr. Smith's ECG Blog
OCTOBER 17, 2024
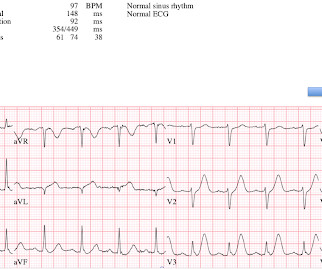
Past medical history included RBBB without other cardiac history, but old ECG was not available. The prehospital and ED computer interpretation was inferior STEMI: There’s normal sinus rhythm, first degree AV block and RBBB, normal axis and normal voltages. Vitals were normal except for oxygen saturation of 94%. Vitals were normal.
Dr. Smith's ECG Blog
OCTOBER 9, 2018
link] In this paper, in a department in which they state they have only 50 STEMI per year, they looked at only 8 days worth of triage ECGs for a total of 538. They did not find one STEMI on their triage ECGs (no surprise! We at HCMC have 30 walk-in STEMIs per year; the rest come by ambulance. Am J Emerg Med 36(10):1771-1774.

Dr. Smith's ECG Blog
DECEMBER 13, 2023
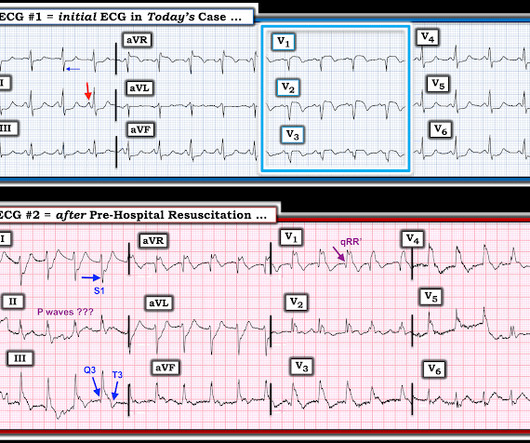
For technical reasons — P waves are not well visible in this tracing — BUT — the P wave in lead I appears to be larger than the P wave in lead II , which is often a tip-off to LA-LL Reversal ( See My Comment in the November 19, 2020 and the May 24, 2022 posts in Dr. Smith's ECG Blog ).
Dr. Smith's ECG Blog
JANUARY 8, 2024
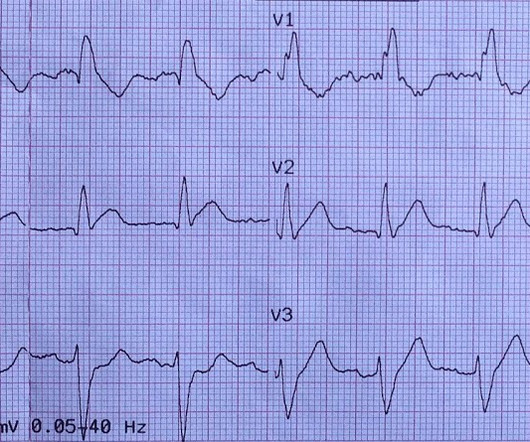
She was diagnosed with a Non-STEMI and kept overnight for a next day angiogram. Medics recorded the above ECG and called a STEMI alert. The patient went into arrest pre-hospital. ECG Findings that Suggest Acute PE: We have presented numerous cases of acute PE in multiple posts in Dr. Smith’s ECG Blog.
Dr. Smith's ECG Blog
NOVEMBER 19, 2014
Here are three more dramatic cases that illustrate RBBB + LAFB Case 1 of cardiac arrest with unrecognized STEMI, died. Furthermore, among 35 patients with acute left main coronary artery occlusion, 9 presented with RBBB (mostly with LAH) on the admission ECG.
Dr. Smith's ECG Blog
FEBRUARY 25, 2009
RBBB in acute STEMI has a very high mortality. Were it not for this prehospital ECG and the cardiac arrest, the diagnosis may have been significantly delayed. Had this happened, the artery may have re-occluded prior to angiography, with resultant recurrent cardiac arrest and/or shock and death.
Dr. Smith's ECG Blog
OCTOBER 11, 2020
The provider contacted cardiology to discuss the case, but cardiology "didn't think it was a STEMI, didn't think he needed emergent cath." About two hours after admission, he suffered a cardiac arrest (whether it was VF/VT or PEA is not available) and expired. The whole paradigm is literally called "STEMI" vs. "NSTEMI."
Dr. Smith's ECG Blog
JUNE 15, 2013
The cath lab was activated for STEMI. Unfortunately, the patient had a cardiac arrest on arrival to the cath lab, before return of the potassium. Hyperkalemia alone can cause inferior-posterior pseudo-STEMI: Notice that in both cases, the ST elevation is downsloping and the T-wave is inverted. The potassium returned at 8.4
Dr. Smith's ECG Blog
NOVEMBER 23, 2022
About an hour later, he was then found on the floor in cardiac arrest in the ED. Sooner identification likely leads to better outcomes, and in this case may have allowed prevention of cardiac arrest and better long-term outcome. His initial troponin T was 15 ng/L (only two hours since pain onset).
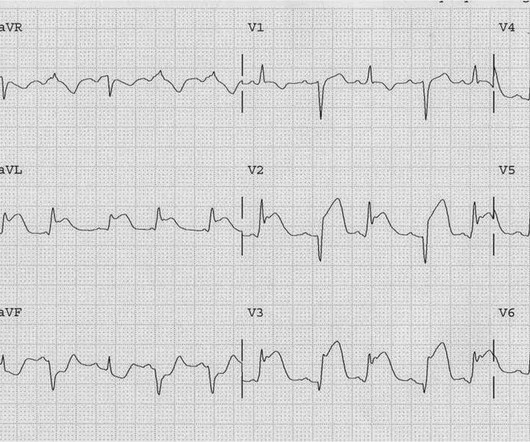
Dr. Smith's ECG Blog
DECEMBER 23, 2014
The patient was diagnosed with esophageal reflux and was being discharged by the nurse when he had a cardiac arrest. Anterolateral STEMI. The formula results in 23.43, just above the 23.4 He was defibrillated. Here is his post resuscitation ECG: Now the diagnosis is obvious.

Dr. Smith's ECG Blog
NOVEMBER 4, 2022
This has been termed a “STEMI equivalent” and included in STEMI guidelines, suggesting this patient should receive dual anti-platelets, heparin and immediate cath lab activation–or thrombolysis in centres where cath lab is not available. aVR ST segment elevation: acute STEMI or not? aVR ST Segment Elevation: Acute STEMI or Not?
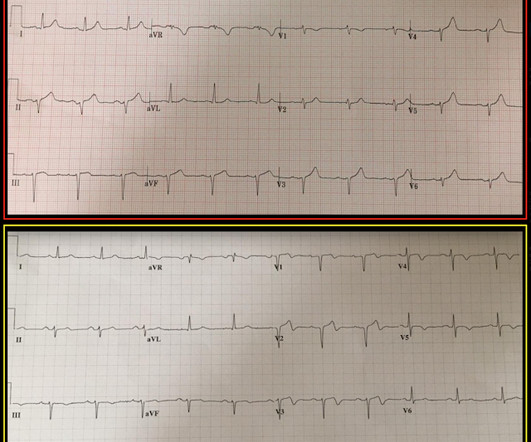
Dr. Smith's ECG Blog
SEPTEMBER 20, 2018
There is a very small amount of STE in some of the anterior, lateral, and inferior leads which do NOT meet STEMI criteria. The case was reviewed by all parties, and it was stated correctly that the ECG does not meet the STEMI criteria. The STEMI vs. NSTEMI paradigm is not the best way to decide who needs emergent reperfusion therapy.
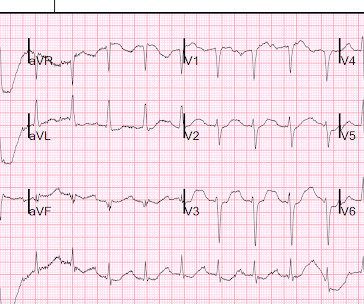
Dr. Smith's ECG Blog
FEBRUARY 2, 2017
Discussion See this post: STEMI with Life-Threatening Hypokalemia and Incessant Torsades de Pointes I could find very little literature on the treatment of severe life-threatening hypokalemia. If cardiac arrest from hypokalemia is imminent (i.e., When the ECG shows the effects of hypokalemia, it is particularly dangerous.

Dr. Smith's ECG Blog
DECEMBER 15, 2015
It was a PEA or bradyasystolic arrest , not a shockable rhythm. Although most cardiac arrest from MI is due to ventricular fibrillation, some is due to high grade AV block, and so this could indeed be due to large acute STEMI. LV anterior STEMI does not give maximal ST elevation in V1. Is this an anterior (LV) MI?

Dr. Smith's ECG Blog
SEPTEMBER 16, 2015
It may be difficult to read STEMI in the setting of RBBB. There is, however, a long QT also, with abnormal T-waves, but this is not STEMI. This ECG was recorded prehospital, and the computer read STEMI, so the medics activated the cath lab: What do you think? The ECG is consistent with high lateral STEMI. Called 911.
Expert insights. Personalized for you.
We have resent the email to
Are you sure you want to cancel your subscriptions?


Let's personalize your content